Research - Clinical Schizophrenia & Related Psychoses ( 2021) Volume 0, Issue 0
The Association Between Serum Levels Of Ferritin And Ddimer With Liver Function Tests In Patients With Covid19
Wisam Abdulameer Noman1, Hanaa Addai Ali1*, Ahmed Beseem Mahdi2, Rahman S Zabibah3 and RawaaAdday Ali42Department of Chemistry, University of Babylon, Hillah, Iraq
3Department of Medical Technology, University of Islami, Najaf, Iraq
4Department of Microbiology, AL-Qasim Green University, AL-Qasim, Iraq
Hanaa Addai Ali, Department of Pharmacology and Toxicology, University of Babylon, Hillah, Iraq, Email: phar.hayder.abdul@uobabylon.edu.iq
Received: 12-Jul-2021 Accepted Date: Jul 26, 2021 ; Published: 02-Aug-2021
Abstract
Background: SARS-CoV-2, the culprit responsible for the 2019 new coronavirus disease (COVID-19), has posed a serious threat to worldwide public health. At the moment, it is estimated that the novel coronavirus severe acute respiratory syndrome corona virus 2 (SARS-CoV-2) has infected It has infected a huge number of people worldwide and is responsible for the clinical syndrome of coronavirus sickness 2019 (COVID-19). Although the primary clinical manifestation is pulmonary disease, mounting evidence supports the involvement of multiple organ systems, including the Gastro Intestinal (GI) tract and liver. To evaluate the potential changes in liver function tests, and their association with illness severity and mortality in patients with COVID-19.
Materials and methods: This case-control study of 90 subjects were included, 60 patients admitted to Merjan Hospital, Babel, Iraq infected with COVID-19 and 30 samples of healthy subjects as a control group. The serum levels of ALT, AST, Alp, and albumin were measured by colorimetric methods. Serum ferritin and d-dimer were measured by ichroma, and CBC conducting a statistical analysis and associated with the severity of disease.
Results: In this study, the results demonstrated a significant increase in levels of ALT, AST, ALP, ferritinin, and D-dimer in patients compared with the healthy group. Levels of serum ferritin have a significant positive correlation with D-dimer, ALP, AST, ALT, and NLR levels. While, it has a significant negative correlated with serum albumin in patients with corona virus group. The neutrophil percentage significantly higher than normal. While, the lymphocyte percentage was significantly lower in patients with elevated ferritin and d-dimer levels than the healthy group.
Conclusion: COVID-19 patients with abnormal liver function testes are common in hospitalized patients with COVID-19, and associated with illness severity and rate of death as a higher incidence of severity illness and liver injury in patients with increased levels of serum ferritin, and D-dimer.
Keywords
Liver injury • Statistical analysis • Coronavirus • Investigation
Introduction
The first case of SARS-CoV-2 viral pneumonia was discovered in Wuhan, Hubei Province, China in December of 2019.Since then, the virus has been spread throughout a world, with a number of documented cases increasing daily [1,2]. The mechanism through which COVID-19-induced liver impairment occurs is unknown. Angiotensin-Converting Enzyme 2 (ACE2) expression in cholangiocytes and hepatocytes has been established as a SARS-CoV-2 receptor [3]. As a result, SARS-CoV-2 is capable of infecting the liver and causing damage. Other researchers believe that liver damage is caused by a cytokine storm. In COVID-19 [4].
Ferritin has identified as a diagnostic or prognostic marker in patients with liver disease. Disorders due to its ability to be generated in the presence of systemic inflammation [5]. Serum ferritin levels had positive associations with blood ALT levels [6]. Patients with COVID-19 had liver comorbidities, and some cases showed abnormal alanine and separate amino transferase levels (AST) [7]. Also of patients with COVID-19 during hospitalization elevated alkaline phosphates levels [3]. Additionally, the reduction in serum albumin levels may be due to moderate diarrhea during the onset of the disease, provided the patients' urine albumin levels are extremely low. As a result, we hypothesize that hepatocyte failure in albumin production is the most likely cause of hypoalbuminemia [8]. The ratio of neutrophils to lymphocytes has been found to be related with the liver function of COVID-19 patients [4]. Elevated D-dimer levels in patients with elevated ALT levels indicate an overactive coagulation/fibrinolysis system; Concurrent elevations in ALT and D-dimer levels show that liver illness may be caused, in part, by intrahepatic circulation problems precipitated by intrahepatic micro vascular thrombosis [9].
Materials and Methods
This case control study of 90subjects was conducted age 40 to 66 years. A total was included 60 confirmed patients with COVID-19 admitted to Merjan Hospital, Babel, Iraq, from the period between January 20th 2020 and April 2021. Patients with COVID-19 were confirmed according to the positive results of quantitative RT-PCR and chest x-ray or CT scan and 30 healthy subjects as a control group whose ages were close to the group of patients. To avoid the influence of other comorbidities, this study excluded subjects with diabetic, Alcoholics, liver disease and smokers.
This investigation was approved by local medical ethics committee and all participants gave informed consent before the onset of study. Also, acceptable by the hospital's administrators from medical records, and gathered demographic information, history of medical, history of exposure, signs and symptoms, and laboratory finding. Venous Blood samples were collected from patients and control groups. Blood samples were separated in to two tubes. 3 ml allowed to clot for 10-15 minutes at room temperature before centrifugation for 10 minutes at (3000 Xg) in order provide serum. Then serum samples were separated in to tubes and stored at -80°C until time of analysis. Remaining blood (2 ml) was prepared to measure complete blood count. The concentrations of serum AST, ALT, ALP, albumin, were measured by using colorimetric methods kits (Cobas, Roche). Serum ferritin and D-dimer levels were measured by fluorescence immunoassay (ichromaTM). Complete blood count was measured by using auto hematology analyzer (linear, Spain).
Statistical Analysis
To verify correctness, each item of data was entered multiple times into a computer in (excel) check mode. Additionally, some values are calculated using formulae. To investigate the relationship between the two groups. And compare to the remaining groupings. The variable was denoted by "mean & (SD)," and the t-test was performed to determine the difference between the groups. For each and every variable. All data were evaluated statistically using "IBM SPSS statistics version 25.0," with significance set at P.05.
Results
In Table 1 summarized the demographic and clinical characteristics in the groups studied, which consist data of serum D-dimer, ferritin, alkaline phosphatase, ALT, AST were significantly higher. But, significantly lower NLR, platelet count albumin in covid-19 patients group when compared with healthy group.
|
Covid-19 patients group Mean ± SD |
Control group Mean ± SD |
|
||
|---|---|---|---|---|---|
| Age(years) | 61.111 ± 7.647 | 58.2601 ± 5.765 | 0.60 | ||
| Male/Female female% male % |
17/13 56.6% 43.4 | 17/13 56.6% 43.4 | |||
| Hb g/dl | 12.74 ± 1.95 | 14.27 ± 0.92 | 0.05 | ||
| Lymphocyte % | 10.57 ± 4.72 | 21.54 ± 5.75 | 6E-11 | ||
| Neutrophil % | 82.16 ± 11.47 | 46.503 ± 10.54 | 4.3E-18 | ||
| NLR | 9.989±6.956 | 2.261 ± 0.629 | 1.27E-06 | ||
| PLT 10^9/l | 274 ± 123 | 360 ± 29.6 | 0.56 | ||
| D-dimer(ng/ml) | 630.4 ± 30.26 | 266.14 ± 20.07 | 0.001 | ||
| Ferritin (ng/ml) | 914.60 ± 608.013 | 105.92 ± 34.739 | 4.94576E-08 | ||
| ALT( IU/L) | 34.23 ± 14.76 | 17.79 ± 2.699 | 0.005622 | ||
| AST (IU/L) | 50.4 ± 22.1 | 25.6 ± 4.4 | 7.6E-05 | ||
| ALP (IU/L) | 167.25 ± 102.513 | 82.933 ± 8.09291 | 0.017636 | ||
| Albumin g/dl | 1.8333 ± 0.986 | 3.4733 ± 0.240 | 5.71E-07 |
Mean ± SD: Standard Deviation, ALT: Alanine Amino Transferase, AST: Aspartate Amino Transferase, ALP: Alkaline Phosphates, NEUT: Neutrophil, LYM: Lymphocyte, PLT: Platelet, NLR: Neutrophil Lymphocyte Ratio.
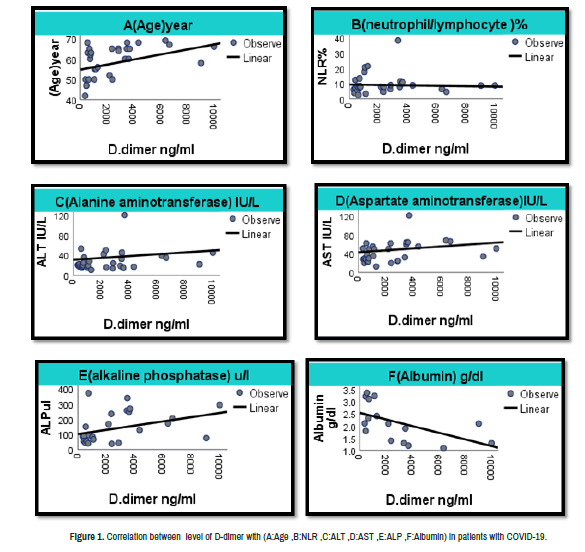
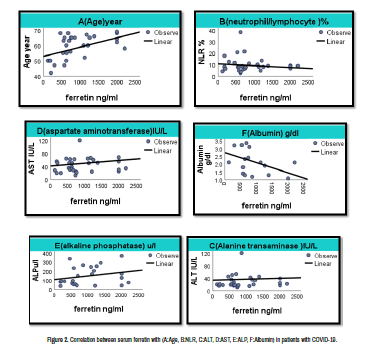
Levels of serum ferritin and D-dimer have a significant positive correlation with age, platelet ALT, AST, ALP. While, it has a significant negative correlated with albumin in patients with corona virus disease 2019 group as shown in Table 2 and Figures 1 and 2.
|
Parameters |
r&P-value | D-dimer (ng/ml) | Ferritin (ng/ml) |
|---|---|---|---|
|
|
R | 467** | 0.527** |
| p-value | 0.009 | 0.003 | |
|
BMI (kg/m2 ) |
r | 521** | 0.229 |
| p-value | 0.003 | 0.223 | |
|
Neutrophils % |
r | 361 | 0.113 |
| p-value | 0.050 | 0.553 | |
|
Lymphocyte % |
r | -0.005 | -0.035 |
| p-value | 0.978 | 0.854 | |
|
NLR |
r | - 0.020 | -0.122 |
| p-value | 0.918 | 0.521 | |
|
Platelet 10^9/l |
r | -0.363** | -0.446** |
| p-value | 0.048 | 0.013 | |
|
ALT ( IU/L) |
r | 0.380 | 0.39 |
| p-value | 0.050 | 0.041 | |
|
Alkaline |
r | 0.354 | 0.236 |
| p-value | 0.050 | 0.267 | |
|
Albumin (g/dl) |
r | -0567** | -0.392** |
|
|
p-value | 0.022 | 0.134 |
|
D-Dimer(ng/ml)
|
|
|
0.595** |
|
|
|
|
0.001 |
|
**: significance set at P .05. |
|||
Discussion
COVID-19 infection often manifests as pulmonary symptoms, however it may also manifest as damage to other organs including as the heart muscle, kidneys, and liver [10]. In this study, we discovered numerous risk variables for liver impairment in COVID-19 patients who were hospitalized. Several significant elements, such as the decreased (albumin, NLR), and increased AST, ALT, d-dimer, ferritin. All were related with an increased risk of liver dysfunction in patients admitted to the hospital. D-dimer levels were found to be significantly higher in our sample than in a healthy control sample, corroborating previously published findings. This evidence suggests that frequent hemostasis testing may be valuable tools for enhancing early detection. Significantly, the continuous escalation of illness severity was reflected in increasing D-dimer readings [11]. We observed that D-dimer rise on admission was prevalent in patients diagnosed to COVID-19 and was linked with greater disease severity and in-hospital mortality. D-dimers are one of the pieces formed when fibrin is cleaved by plasmin to dissolve clots [12]. Given the contemporaneous increase in D-dimer and ALT levels despite heparin therapy, it is likely that liver dysfunction was caused, at least in part, by intrahepatic micro vascular thrombosis following pulmonary embolism [13]. SARS-CoV and SARS-CoV-2 both enter the host cell via the ACE2 receptor. Both bile duct cells and hepatocytes produce ACE2, which may explain why SARSCoV-2 infection results in liver impairment [3]. Although people with severe of COVID-19 may have elevated levels of d-dimer, creatinine, or brain natriuretic peptide. The precise association between liver injury and coagulation system, renal, or heart attack is still unknown [14]. There is a correlation between albumin and D-dimer levels in COVID-19, with the latter being a well-established marker of thrombotic risk and higher mortality [15].
In several studies, patients with COVID-19 were identified and baseline features of individuals with elevated and normal ferritin levels were estimated. When compared to ferritin alone, the combined models didn’t significantly increase diagnostic capacities for COVID-19 severity disease or liver disease demonstrating that ferritin may function as a selfsufficient, easy-to-use signal. Additionally, another study compared the viral clearance rate and length of hospital stay in patients with high ferritin levels in comparison to people with normal ferritin levels and revealed that ferritin was a predictive factor for COVID-19 patient prognosis. Thus, it is possible to hypothesize that ferritin could be an effective discriminator of liver injury, disease severity, and prognosis [16,17]. Serum ferritin has been long studied as a marker of iron metabolism [18]. However, its use as an inflammatory biomarker has been established to be critical in the context of COVID-19 advancement in prior studies in the field [19]. Ferritin is an acute phase reactant, and as such, it is frequently increased during all types of inflammatory responses.
In some patients, COVID-19 infection can result in liver injury. Elevated liver function indicator levels, such as ALT, AST, ALP, and T BiL, were associated with an increased mortality risk associated with COVID-19 infection [20]. Currently, only a few researchers have documented a significant increase in serum ALP levels during COVID-19 infection. The current investigation discovered that the median levels of ALP exhibited an upward trend, with a considerable increase in the median levels of ALP in severe cases. A part from the consequences of aging, high ALP levels may indicate bile duct damage [21]. Hypoalbuminemia can occur as a result of liver disease. In critical patients, hypoalbuminemia and increased AST levels were frequently detected, and a link between albumin and AST levels and illness severity was also discovered [22]. In non-severe cases, liver impairment was modest and transitory. The primary conclusion is that elevated AST levels were more frequent and significant in severe patients admitted to the hospital than increased ALT levels, and AST levels showed the highest link with death when compared to other indications of liver impairment [23].
This contradicts other reports of hepatitis-associated liver damage. ALP levels considerably increased toward the end of the disease but remained generally within the normal range [24]. Increased ALT, AST, ALP, and TBIL levels were related with an increased risk of death, with higher AST having the highest mortality risk among these liver enzymes. Increased signs of liver injury were usually associated with a decrease in lymphocyte count, an increase in neutrophil count, and male gender [25].
Conclusion
The higher levels of D-dimer and ferritin independently associated with an increase levels of liver function tests. That the possible coagulopathy is associated with liver injury produced by micro vascular thrombosis in addition to systemic inflammation. Some COVID19 patients who suffer liver failure may acquire systemic coagulopathy, increasing their likelihood of developing severe disease. And, these findings indicate that early ferritin testing may be an effective tool for diagnosing liver injury, illness severity, and a bad prognosis in COVID-19 patients. The mechanisms behind the liver damage induced by SARS-CoV-2 infection are mostly unclear. Our current understanding indicates that infection with a highly pathogenic human coronavirus may produce liver injury through virus-induced cytopathology and immunopathology caused by excessive inflammatory responses.
Acknowledgements
The authors thank the patients for their cooperation and the medical staffs in the laboratories in Life Center and Healing at Marjan Medical Hospital in Babylon Governorate for cooperation in collecting the samples and for perform the required laboratory tests.
Conflict of Interest
The authors declare that they have no conflict of interest.
Funding
Self-funding.
Ethical Consideration
All Participants passed informed agreement, consistent with the protocol permitted by the Local Institutional Ethics Committee.
References
- Cao, Peng, Sanlan Wu, Tingting Wu, and Yahui Deng, et al. “Since January 2020 Elsevier Has Created a COVID-19 Resource Centre with Free Information in English and Mandarin on the Novel Coronavirus COVID- 19.” 3 (2020): 1-7.
- Han, Chaoqun, Caihan Duan, Shengyan Zhang, and Brennan Spiegel, et al. “Digestive Symptoms in COVID-19 Patients With Mild Disease Severity.” Am J Gastroenterol 115 (2020): 916–23.
- Chai, Xiaoqiang, Longfei Hu, Yan Zhang, and Weiyu Han, et al. “Specific ACE2 Expression in Cholangiocytes May Cause Liver Damage After 2019-nCoV Infection.” biorxiv 5 (2020):1-13.
- Zhang, Chao, Lei Shi, and Fu Sheng Wang. “Liver Injury in COVID-19: Management and Challenges.” Lancet Gastroenterol Hepatol 5 (2020): 428–30.
- Jung, Ju Young, Jae-Jun Shim, Sung Keun Park, and Jae-Hong Ryoo, et al. “Serum Ferritin Level is Associated with Liver Steatosis and Fibrosis in Korean General Population.” Hepatol Int 13 (2019): 222-233.
- Kowdley, Kris V, Patricia Belt, Laura A Wilson, and Matthew M Yeh, et al. “Serum Ferritin is an Independent Predictor of Histologic Severity and Advanced Fibrosis in Patients with Nonalcoholic Fatty Liver Disease.” Hepatology 55 (2012): 77-85.
- Huang, Chaolin, Yeming Wang, Xingwang Li, and Lili Ren, et al. “Clinical Features of Patients Infected with 2019 Novel Coronavirus in Wuhan, China.” Lancet 395 (2020): 497–506.
- Murthy, Srinivas, Charles D Gomersall, and Robert A Fowler.“Care for Critically ill Patients with COVID-19.”Jama 323 (2020): 1499-1500.
- Ackermann, Maximilian, Stijn E Verleden, Mark Kuehnel, and Axel Haverich, et al.“Pulmonary Vascular Endothelialitis, Thrombosis, and Angiogenesis in Covid-19.”N Engl J Med 383 (2020): 120-128.
- Li, Qun, Xuhua Guan, Peng Wu, and Xiaoye Wang, et al. “Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus–Infected Pneumonia.” N Engl J Med 382 (2020): 1199–1207.
- Fu, Jianhong, Jindan Kong, Wei Wang, and Meiying Wu, et al. “The Clinical Implication of Dynamic Neutrophil to Lymphocyte Ratio and D-dimer in COVID-19: A Retrospective Study in Suzhou China.” Thromb Res 192 (2020): 3-8.
- Linkins, L‐A, and S Takach Lapner.“Review of D‐dimer Testing: Good, Bad, and Ugly.” Int J Lab Hematol 39 (2017): 98-103.
- Tsutsumi, Takeya, Makoto Saito, Hiroyuki Nagai, and Shinya Yamamoto, et al.“Association of Coagulopathy with Liver Dysfunction in Patients with COVID‐19.” Hepatol Res 51 (2021): 227-232.
- Qin, Chuan, Luoqi Zhou, Ziwei Hu, and Shuoqi Zhang, et al.“Dysregulation of Immune Response in Patients with Coronavirus 2019 (COVID-19) in Wuhan, China.”Clin Infect Dis 71 (2020): 762-768.
- Basili, Stefania, Roberto Carnevale, Cristina Nocella, and Simona Bartimoccia, et al.“Serum Albumin is Inversely Associated with Portal Vein Thrombosis in Cirrhosis.” Hepatol Commun 3 (2019): 504-512.
- Chen, Xiaoping, Wenjia Hu, Jiaxin Ling, and Pingzheng Mo, et al. Hypertension and Diabetes Delay the Viral Clearance in COVID-19 Patients”. Medrxiv 10 (2020): 1-12.
- Cao, Peng, Yu Zhang, Zi Huang, and Mitchell A Sullivan, et al. “The Preventative Effects of Procyanidin on Binge Ethanol‐Induced Lipid Accumulation and ROS Overproduction Via the Promotion of Hepatic Autophagy.” Mol Nutr Food Res 63 (2019): 1970045.
- Kell, Douglas B, and Etheresia Pretorius. “Serum Ferritin is an Important Inflammatory Disease Marker, as it is Mainly a Leakage Product from Damaged Cells.” Metallomics 6 (2014): 748-773.
- Henry, Brandon Michael, Maria Helena Santos De Oliveira, Stefanie Benoit, and Mario Plebani, et al. “Hematologic, Biochemical and Immune Biomarker Abnormalities Associated with Severe Illness and Mortality in Coronavirus Disease 2019 (COVID-19): A Meta-Analysis.” Clin Chem Lab Med 58 (2020): 1021-1028.
- Lei, Fang, Ye‐Mao Liu, Feng Zhou, and Juan‐Juan, et al. “Longitudinal Association between Markers of Liver Injury and Mortality in COVID‐19 in China.” Hepatology 72 (2020): 389-398.
- Hoffmann, Markus, Hannah Kleine-Weber, Nadine Krüger, and Marcel Müller, et al. “The Novel Coronavirus 2019 (2019-nCoV) Uses the SARS-Coronavirus Receptor ACE2 and the Cellular Protease TMPRSS2 for Entry into Target Cells.” BioRxiv 181 (2020):271-280.
- Lei, Ping, Lan Zhang, Ping Han, and Chuansheng Zheng, et al.“Liver Injury in Patients with COVID-19: Clinical Profiles, CT Findings, the Correlation of the Severity with Liver Injury.”Hepatol Int 14 (2020): 733-742.
- Xu, Zhe, Lei Shi, Yijin Wang, and Jiyuan Zhang, et al.“Pathological Findings of COVID-19 Associated with Acute Respiratory Distress Syndrome.”Lancet Respir Med 8 (2020): 420-422.
- Yang, Xiaobo, Yuan Yu, Jiqian Xu, and Huaqing Shu, et al. “Clinical Course and Outcomes of Critically Ill Patients with SARS-CoV-2 Pneumonia in Wuhan, China: A Single-Centered, Retrospective, Observational Study.” Lancet Respir Med 8 (2020): 475–81.
- Zhang, Yafei, Liang Zheng, Lan Liu, and Mengya Zhao, et al.“Liver Impairment in COVID‐19 Patients: A Retrospective Analysis of 115 Cases from a Single centre in Wuhan City, China.” Liver Int 40 (2020): 2095-2103.
Citation: Noman Wisam, Abdulameer, Hanaa Addai Ali, Ahmed Beseem Mahdi, and Rahman S Zabibah et al. "The Association between Serum Levels of Ferritin and D-Dimer with Liver Function Tests in Patients with COVID-19" Clin Schizophr Relat Psychoses 15S(2021). Doi:10.3371/CSRP.NWAH.072821.
Copyright: © 2021 Norman WA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.