Research Article - Clinical Schizophrenia & Related Psychoses ( 2022) Volume 0, Issue 0
Post Stroke Fatigue Prevalence and its Correlation to the Functional Recovery
Ahmed S. Ali1*, Dania S.Farid1, Wael S. Shendy1, Husam S.Mourad2, Khaled Takey Ahmed3, Waleed Elsayed Hussein Ahmed Arafat4 and Ayman El Khatib52Department of Neurology, Cairo University, Egypt
3Department of Physical Therapy for Cardiopulmonary and Geriatrics, Misr University for Sciences and Technology, Egypt
4Department of Physical Therapy for Cardiovascular and Geriatrics, Egyptian Chinese University, Cairo, Egypt
5Department of Physical Therapy, Beirut Arab University, Beirut, Lebanon
Ahmed S. Ali, Department of Physical Therapy for Neuromuscular Disorders and its Surgery, Cairo University, Cairo, Egypt, Email: Dr.shawky_2011@cu.edu.eg
Received: 28-Jan-2022, Manuscript No. CSRP-22-52822; Editor assigned: 31-Jan-2022, Pre QC No. CSRP-22-52822 (PQ); Reviewed: 14-Feb-2022, QC No. CSRP-22-52822; Revised: 21-Feb-2022, Manuscript No. CSRP-22-52822 (R); Published: 28-Feb-2022, DOI: 10.3371/CSRP.AADF.022822
Abstract
Background: Post Stroke Fatigue (PSF) is an irritating symptom in chronic stroke survivors. They report that the symptoms of the PSF are greater after their stroke’s incidence which might affect the rehabilitation process. PSF could limit the active participation of the patient in the environment as well as in different functional tasks of daily living activities.
Purpose: To determine the PSF prevalence in chronic stroke patients and to investigate its correlation on their functional recovery.
Materials and methods: One hundred Egyptian chronic stroke patients participated in this study from both sexes. All the patients aged between 40 to 65 years. They were recruited from the outpatient clinics of The Faculty of Physical Therapy, Cairo University. Demographic data were collected (age, sex). Post Stroke Fatigue was evaluated by using the Arabic validated versions of both the Fatigue Severity Scale (FSS) and the Modified Fatigue Impact Scale (MFIS). The functional recovery was evaluated by the Barthel’s Index (BI). The demographic data was assessed, and the functional recovery was correlated to the outcome measures of the PSF.
Results: The prevalence of PSF in stroke patients was 62% using the FSS and 66% using the MFIS. There was a significance increase in the severity and the impact of PSF in the females (p<0.05). The correlation between BI and FSS was a significant moderate negative correlation (r=-0.42, p=0.0001) and between BI and MFIS was a significant moderate negative correlation (r=-0.50, p=0.0001).
Conclusion: PSF is moderately prevalent among chronic stroke patients with 62% using the FSS and 66% using the MFIS. PSF is significantly prevalent in the females more than the male stroke survivors. It has a moderate negative significant correlation to the patient’s functional recovery. This indicates that the patient’s ability to act independently in different functional activities could be related to the presence and the severity of the PSF. It could act as one of the barriers for the stroke survivors to their physical recovery.
Keywords
Post stroke fatigue • Fatigue severity scale • Modified fatigue impact scale • Barthel index • Functional recovery
Introduction
Stroke is considered clinically as fast developed signs of focal or global disturbance of cerebral function that last for twenty-four hours or more [1]. It increased worldwide in both sexes of different ages [2]. In the last ten years, stroke was considered as the second leading cause of death where hypertension is the main risk factor for its incidence [3], as well as the psychological and the emotional stresses [4]. Other risk factors could take place as diabetes mellitus, smoking, hyperlipidaemia, obesity, poor diets and decreased physical activity [5,6].
Cognitive dysfunctions are considered as an important sign in stroke which increases and becomes severe in stroke’s recurrence [7]. They are presented as features of a decreased attention, problems in execution of functional tasks, impairments of the memory and language and perceptual disorders of the affected side [8]. Fatigue, cognitive dysfunctions, and psychological impairments were reported to be presented in 20%-50% of stroke patients which have a negative impact on their lives [9]. The persistence of the fatigue symptoms may affect the cognitive abilities of stroke patients as well as the psychological status [10].
Fatigue is considered as the awareness of a decreased capacity of physical or mental functions. The origin of fatigue could be peripheral of short duration or central of longer duration. Peripheral fatigue is a normal response that takes place in the healthy subjects after a severe physical activity. It involves a dysfunction of the peripheral nervous system as impaired neuromuscular transmission at the motor end plate which decreases by rest or sleep. Central fatigue is the pathological form; it usually happens with a psychological origin or associated with an underlying pathology as cancer, multiple sclerosis, and stroke [11].
Post Stroke Fatigue (PSF) involves a dysfunction of the central nervous system due to impairment in the transmission between it and the peripheral nervous system. It is reported that the hypothalamic region could be affected besides other areas in the cortex [12] and a disturbance in the somatosensory feedback mechanism as the higher brain centres cannot control the drive of production of the functional outcomes [13].
The PSF is presented soon after stroke’s onset and remains common in the longer term which has economic and psychological effects since it prevents individuals of good recovery from returning to their jobs [14,15]. They report of being more fatigued than before the stroke. This threatens their physical functions as well as the quality of life [16]. It can become more severe, and it is associated with an increased fatality and mortality. It does not receive big attention from the healthcare providers [17,18].
It is recommended that further research needed to understand its time course, associations [19], etiology and pathogenesis to manage its symptoms [20]. The main domains and characteristics of PSF remain poorly investigated through the literature [21,22]. The information available to target both the etiology and the pathogenesis are limited [21,23].
Materials and Methods
Subjects
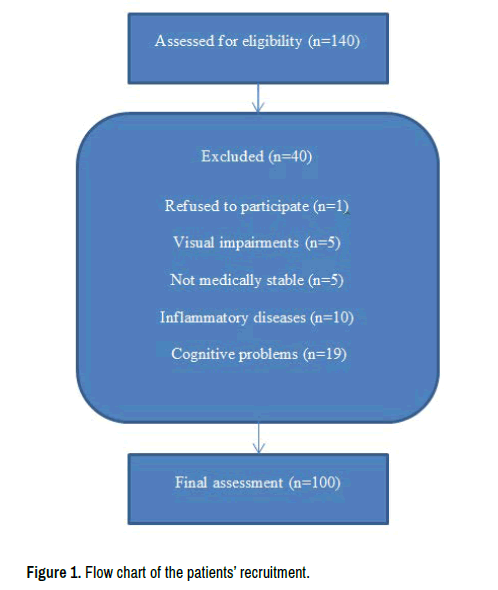
One hundred and forty patients met the inclusion criteria of the study. One patient refused to participate in the study. Five patients had visual impairments. Five patients were not medically stable (active cancers, history of seizures). Ten patients had an inflammatory disease (severe arthritis), and nineteen patients were excluded for cognitive problems using the Arabic validated version of the Mini Mental Status Examination Scale (MMSE). Total patients recruited in the study were one hundred patients; the flow chart of the recruited patients is described in Figure 1.
Inclusion criteria
Chronic ischemic stroke, age of the recruited patients ranged from 40 and 65 years, duration of stroke was six months or more, ambulant patients, medically stable patients, patients could follow the oral commands and were free from any secondary complications such musculoskeletal or neuromuscular disorders. The patients were recruited from the outpatient clinic of the Faculty of Physical Therapy, Cairo University after being diagnosed by a neurologist and confirmed by a Computed Topography Scan (C.T scan). The study was conducted in outpatient clinic of The Faculty of Physical Therapy, Cairo University from July 2019 till January 2020 and was granted the approval of the Research Ethical Committee of the Faculty of Physical Therapy–Cairo University (Approval NO: P.T.REC/012/002154).
Exclusion criteria
Pregnant patients, patients with cognitive dysfunctions or having inflammatory or infectious diseases, patients with other neurological deficits or orthopaedics abnormalities such as contractures, neuropathies, myopathies, fractures, trauma, or deformities and patients with history of seizures, cardiovascular or pulmonary diseases or having visual impairments did not participate in this current study.
Procedures
The study design was cross sectional study. The primary outcomes recorded were as follows: Arabic validated versions of both Fatigue Severity Scale (FSS) (24) Modified Fatigue Impact Scale (MFIS) (25) were recorded to assess Post Stroke Fatigue (PSF) and Barthel Index (BI) used to assess functional recovery post stroke [24,25].
The FSS is a nine-item questionnaire that only detects the severity of the fatigue [26,27], while the MFIS has twenty-one items of three domains which are physical functioning (nine items), cognitive functioning (ten items), and psychosocial functioning (two items) which were selected by the National Multiple Sclerosis Society Council [28,29]. Barthel Index (BI) measures the individual’s performance in 10 different and selected functions of activities of daily living. The values assigned to each item in the BI are based on the amount of physical assistance required to perform the task. The items are summed to give a score that ranges from 0 to 100 that indicated the level of independency.
Each subject was asked to sign a form of consent after their approval to join this study after receiving all the information about the aims of this study, procedures, privacy, the use of the data taken and their rights to withdraw from the study whenever they want. The whole procedures of the study were explained to each patient. A clinical assessment was done from each patient and included the muscle tone, the muscle power, the balance, superficial and deep sensations, and reflexes. The demographic data: age and the sex as the independent variables were recorded as the baseline data and were correlated to the outcome variables. The Arabic validated version of Mini-Mental State Examination was used in this study to exclude the chronic stroke patients with cognitive impairments to avoid mental fatigue.
For assessment of post stroke fatigue, each patient had a copied sample to be filled of each scale. Each item was read carefully to the patient. The method of scoring of the FSS is recorded by calculating the mean score of each item. The mean score of 4 or more revealed post stroke fatigue. The total score of the MFIS ranges from 0 to 84. A total score of 38 was the cut off to discriminate fatigued from non-fatigued individuals.
For assessment of functional recovery post stroke, Barthel Index was recorded for each patient. Barthel Index consists of 10 components which are chair and bed transfers, ambulation and wheelchair ambulation, stair climbing, toilet transfers, bowel control, bladder control, dressing grooming and feeding. Each component has 5 items to describe the level of function and participation.
A total BI score of 0-20 suggests total dependence, 21-60 severe dependence, 61-90 moderate dependence and 91-99 slight dependence and 100 severe dependence. The therapist in charge, one of the authors, an MSc in physical therapy for neuromuscular disorders and expert in stroke evaluation and rehabilitation.
Statistical analysis
The statistical analysis was conducted by using statistical SPSS Package program version 20 for Windows (SPSS, Inc., Chicago, IL). Numerical data descriptive statistics including the mean and standard deviation for age, FSS, MFIS, and BI. Categorical data descriptive statistics including the number and percentage for gender, FSS, MFIS, and BI. Chi-square test to compare the relation between gender with FSS, MFIS, and BI. Spearman rank correlation coefficient was used for relation between BI with FSS and MFIS. All statistical analyses were significant at 0.05 level of probability (P ≤ 0.05).
Results
The total number of patients recruited were 100 patients of age group of 40 to 65 year (n=100). The total number of the females were 28 patients (n=28) and the total number of the males were 72 (n=72) patients. The mean age of the total patients was 56.42 and the standard deviation (SD) was 6.16. By evaluating the mean of the FSS, MFIS and the BI in the whole study group, it was revealed to be 38.78, 49.21 and 83.91 respectively. The SD was revealed to be 15.06, 21.23 and 14.75 respectively. The functional disability distribution by Barthel Index (BI) score in the study group revealed that 10 (10.00%) subjects had severe dependence, 48 (48.00%) moderate dependence, 34 (34.00%) slight dependence, and 8 (8.00%) independent.
The statistical analysis by Chi-square test (X2-test) revealed that there was significantly difference (P=0.033; P<0.05) between the prevalence of post stroke fatigue of FSS and gender. So, the prevalence of post stroke fatigue in stroke patients increased in females (78.60%) compared to males (55.60%) within study group and revealed that there was significantly difference (P=0.035; P<0.05) between the prevalence of post stroke fatigue of MFIS and gender. So, the prevalence of post stroke fatigue in stroke patients increased in females (82.10%) compared to males (59.70%) within study group.
The prevalence of PSF according to FSS and MFIS in study group (Table 1), the prevalence of PSF distribution between females and males in study group and the correlation between BI with FSS and MFIS (Tables 2 and 3).
| Scale | Fatigue | Number (%) | Mean ± SD | 95% CI |
|---|---|---|---|---|
|
FSS (n=100) |
Fatigued (>36) |
62 (62.00%) |
48.60 ± 8.25 |
46.50–50.69 |
|
Non fatigued (<36) |
38 (38.00%) | |||
|
MFIS (n=100) |
Significant impact (>38) |
66 (66.00%) |
62.15 ± 11.54 |
58.61–65.68 |
|
Non-significant impact (<38) |
34 (34.00%) |
Table 2: The prevalence of PSF distribution between females and males in study group.
| Gender | FSS | MFIS | ||
| Fatigued (>36) | Non-fatigued (<36) | Fatigued (>38) | Non-fatigued (<38) | |
| Females (n=28) | 22 (78.60%) | 6 (21.40%) | 23 (82.10%) | 5 (17.90%) |
| Males (n=72) | 40 (55.60%) | 32 (44.40%) | 43 (59.70%) | 29 (40.30%) |
| Chi-square value (X2-value) | 4.533 | 4.516 | ||
| P-value | 0.033 | 0.035 | ||
| Significance (P<0.05) | S | S | ||
| Item | Fatigue measurement | r | P-value | Significance |
| Barthel Index (BI) | FSS | -0.42 | 0.0001 | S |
| MFIS | -0.50 | 0.0001 | S |
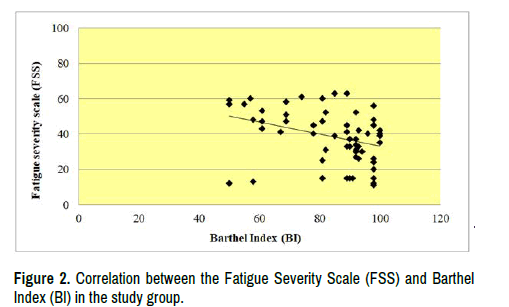
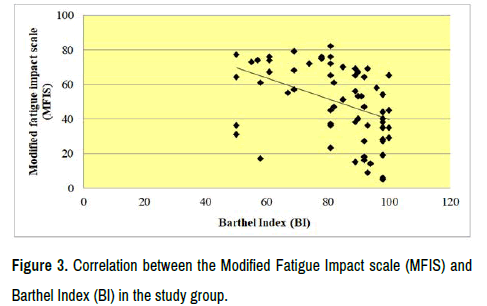
The correlation between the FSS and the BI was revealed to be a moderate negative correlation where r=-0.42 as described in Figure 2. The correlation between the MFIS and the BI was also revealed to be a moderate negative correlation where r=-0.50 as described in Figure 3.
Discussion
The results of this study revealed that the PSF was prevalent among chronic stroke patients with 62% by using the FSS and 66% by using the MFIS. Using more than one scale to assess different domains of the PSF is recommended to avoid bias [30]. There was a significant increase in the severity and the impact of the post stroke fatigue in the females compared with that in the males. The correlation between the PSF and the functional recovery was moderate negative correlation.
The results of the current study agreed with the systematic reviews by Ponchel [31], and Hinkle et al. [32], who justified that the PSF was more frequent in the females due to having more psychological disturbances as depression and anxiety. These disturbances are correlated directly with the PSF symptoms [33].
The results of the current study come with an agreement with Schepers et al. [34], who proved that PSF was prevalent in their sample recruited. It was prevalent at six months and twelve months in 64.1%, and 69.5% respectively with more significant impact on the females which concluded that the PSF is a time dependent factor.
The results of the current study come with an agreement with a review by Nadarajah and Goh [23], who proved that the PSF has a prevalence rates that could reach up to 70% among chronic stroke patients. It was also reported that the severity of the PSF had a significant correlation with the rates of the physical recovery.
The studies done by Vincent-onabajo and Adamu come with an agreement with the current study [35]. They reported that the PSF is prevalent among chronic stroke survivors in their study group which recommended the rehabilitation team to have both awareness and education to address the PSF symptoms in the chronic stroke patients to encourage for more patient participation in the rehabilitation programs.
The current study comes with an agreement with Duncan et al. who reported that the prevalence rates were 66% at six months and 64% at twelve months since stroke’s incidence with a significant negative correlation between the PSF and the domains of the functional activity [36].
The results of the current study proved that there was a moderate negative correlation between the central fatigue and the functional recovery which come with an agreement to a review performed by Staub and Bogousslavsky [37]. They suggested that the post stroke fatigue affected the functional abilities. They confirmed that the there was a significant correlation between post stroke fatigue and brainstem and thalamic lesions. This suggests that fatigue may be linked to the interruption of neural networks involved in tonic attention, such as the reticular activating system and would affect the rates of the functional recovery. It was justified that the post stroke fatigue might present with activities that needs a sustained effort.
The current study comes with a disagreement to Appelros [38], who reported that there was no significant association between the sex and the PSF. It was justified that the non-medically stable patients of higher risks as heart diseases and pulmonary diseases were not excluded.
The current study comes with a disagreement to Park et al. who reported that the PSF was prevalent by 30% in chronic stroke patients [39]. It was justified that there were no significant association between it and the functional recovery and the activities of daily living. This was justified by the combination of an organic brain lesion and the inappropriate coping with a new life situation after the stroke leading to PSF.
The results of the current study come with a disagreement to Snaphaan et al. who suggested that the PSF is prevalent by 33% after eighteen months of follow up without functional impairments measured by Barthel Index and Modified Rankin Scale [40]. It is justified that the age was not controlled in the study group and recruiting many young stroke survivors affected the results.
The results of the current study come with a disagreement with Sarfo et al. who reported the prevalence of PSF to be 58.9% at three months and declined to 23.6% at the chronic stage measured during the ninth month since stroke’s incidence [41]. This indicated that it is not highly prevalent in the chronic stage. Another studies performed by Becker et al. and Graber et al. indicated the low prevalence rates in the chronic stage [42,43]. The limitation of these studies is the recruitment of small sample sizes.
Conclusion
It was concluded that the PSF is moderately prevalent among chronic stroke patients. The PSF is significantly prevalent in the females more than the male stroke survivors. The PSF has a moderate negative significant correlation to the patient’s functional recovery. The results of the current study proved that the PSF symptoms may exist in patients with good participation in their ADLs. This also could suggest engaging easier and less complicated functional activities during the rehabilitation sessions to help the patients actively participate in the environment and reach the functional independency.
Limitations
The limitation of the current study was the lack of translated Arabic validated versions to measure and evaluate the PSF symptoms. There were only two scales translated to Arabic were found in the literature and were used in this study. The availability of more scales would enable us to understand the fatigue symptoms in the Arabic speaking cultures.
Funding
This study was not funded by any source.
Declaration of Competing Interests
The authors declare no conflict of interest.
Acknowledgment
Authors would like to acknowledge all stroke patients participating in the study.
References
- Abbott, Anne L., Mauro Silvestrini, Raffi Topakian and Jonathan Golledge, et al. "Optimizing the Definitions of Stroke, Transient Ischemic Attack, and Infarction for Research and Application in Clinical Practice." Front Neurol 8 (2017): 537.
[Crossref] [Google scholar] [pubmed]
- Feigin, Valery L., Mohammad H. Forouzanfar, Rita Krishnamurthi and George A. Mensah, et al. "Global and Regional Burden of Stroke During 1990–2010: Findings from the Global Burden of Disease Study 2010." Lancet 383 (2014): 245-55.
[Crossref] [Google scholar] [pubmed]
- Pistoia, Francesca, Simona Sacco, Diana Degan and Cindy Tiseo, et al. "Hypertension and Stroke: Epidemiological Aspects and Clinical Evaluation." High Blood Press Cardiovasc Prev 23 (2016): 9-18.
[Crossref] [Google scholar] [pubmed]
- Kotlęga, Dariusz, Monika Gołąb-Janowska, Marta Masztalewicz and Sylwester Ciećwież, et al. "The Emotional Stress and Risk of Ischemic Stroke." Neurol Neurochir Pol 50 (2016): 265-70.
[Crossref] [Google scholar] [pubmed]
- Guzik, Amy, and Cheryl Bushnell. "Stroke Epidemiology and Risk Factor Management." Continuum (Minneap Minn) 23 (2017): 15-39.
[Crossref] [Google scholar] [pubmed]
- Benjamin, Emelia J., Salim S. Virani, Clifton W. Callaway and Alanna M. Chamberlain, et al. "Heart Disease and Stroke Statistics—2018 Update: A Report from the American Heart Association." Circulation 137 (2018): e67-e492.
[Crossref] [Google scholar] [pubmed]
- Coco, Daniele Lo, Gianluca Lopez and Salvatore Corrao. "Cognitive Impairment and Stroke in Elderly Patients." Vasc Health Risk Manag 12 (2016): 105-16.
[Crossref] [Google scholar] [pubmed]
- Jokinen, H., S. Melkas, R. Ylikoski and T. Pohjasvaara, et al. "Post‐stroke Cognitive Impairment is Common Even after Successful Clinical Recovery." Eur J Neurol 22 (2015): 1288-94.
[Crossref] [Google scholar] [pubmed]
- Lanctôt, Krista L., M. Patrice Lindsay, Eric E. Smith and Demetrios J. Sahlas, et al. "Canadian Stroke Best Practice Recommendations: Mood, Cognition and Fatigue Following Stroke, Update 2019." Int J Stroke 15 (2020): 668-88.
[Crossref] [Google scholar] [pubmed]
- Van Rijsbergen, Mariëlle WA, Ruth E. Mark, Willem J. Kop and Paul LM De Kort, et al. "Course and Predictors of Subjective Cognitive Complaints During the First 12 Months after Stroke." J Stroke Cerebrovasc Dis 29 (2020): 104588.
[Crossref] [Google scholar] [pubmed]
- Swain, Mark G. "Fatigue in Chronic Disease." Clin Sci 99 (2000): 1-8.
[Crossref] [Google scholar] [pubmed]
- Bhat, Sushanth and Sudhansu Chokroverty. "Fatigue in Neurologic Disorders." Sleep Med Clin 8 (2013): 191-212.
- McMorris, Terry, Martin Barwood and Jo Corbett. "Central Fatigue Theory and Endurance Exercise: Toward an Interoceptive Model." Neurosci Biobehav Rev 93 (2018): 93-107.
[Crossref] [Google scholar] [pubmed]
- Duncan, Fiona, Simiao Wu and Gillian E. Mead. "Frequency and Natural History of Fatigue after Stroke: A Systematic Review of Longitudinal Studies." J Psychosom Res 73 (2012): 18-27.
[Crossref] [Google scholar] [pubmed]
- Andersen, G., D. Christensen, M. Kirkevold and S. P. Johnsen. "Post‐stroke Fatigue and Return to Work: A 2‐year Follow‐up." Acta Neurol Scand 125 (2012): 248-53.
[Crossref] [Google scholar] [pubmed]
- Bendz, Mona. "The First Year of Rehabilitation after a Stroke–from Two Perspectives." Scand J Caring Sci 17 (2003): 215-22.
[Crossref] [Google scholar] [pubmed]
- Glader, Eva-Lotta, Birgitta Stegmayr and Kjell Asplund. "Poststroke Fatigue: A 2-year Follow-up Study of Stroke Patients in Sweden." Stroke 33 (2002): 1327-33.
[Crossref] [Google scholar] [pubmed]
- Alahmari, Wafa, Ahmed Alhowimel, Mazyad Alotaibi and Eirini Kontou, et al. "Physiotherapy Research Society Meeting abstracts." IJTR 25 (2019): 12968.
[Crossref] [Google scholar]
- Das, Abhay K., Paul Willcoxson and Oliver J. Corrado. "Does Long-term Warfarin Affect the Quality of Life of Older People?." Age Ageing 34 (2005): 312-3.
[Crossref] [Google scholar] [pubmed]
- Penner, Iris-Katharina and Friedemann Paul. "Fatigue as a Symptom or Comorbidity of Neurological Diseases." Nat Rev Neurol 13 (2017): 662-75.
[Crossref] [Google scholar] [pubmed]
- Eilertsen, Grethe, Heidi Ormstad and Marit Kirkevold. "Experiences of Poststroke Fatigue: Qualitative Meta‐synthesis." J Adv Nurs 69 (2013): 514-25.
[Crossref] [Google scholar] [pubmed]
- Thomas, Karen, Chloe Gamlin, Anna De Simoni and Ricky Mullis, et al. "How is Poststroke Fatigue Understood by Stroke Survivors and Carers? A Thematic Analysis of an Online Discussion Forum." BMJ Open 9 (2019): e028958.
[Crossref] [Google scholar] [pubmed]
- Nadarajah, Mohanasuntharaam and Hui-Ting Goh. "Post-stroke Fatigue: A Review on Prevalence, Correlates, Measurement, and Management." Top Stroke Rehabil 22 (2015): 208-20.
[Crossref][Google scholar] [pubmed]
- Al-Sobayel, Hana I., Hind A. Al-Hugail, Ranyah M. AlSaif and Nada M. Albawardi, et al. "Validation of an Arabic Version of Fatigue Severity Scale." Saudi Med J 37 (2016): 73-8.
[Crossref] [Google scholar] [pubmed]
- Khalil, Hanan, Alham Al-Shorman, Alia A. Alghwiri and Nour Abdo, et al. "Cross Cultural Adaptation and Psychometric Evaluation of an Arabic Version of the Modified Fatigue Impact Scale in People with Multiple Sclerosis." Mult Scler Relat Disord 39 (2020): 101878.
[Crossref] [Google scholar][pubmed]
- Krupp, Lauren B., Nicholas G. LaRocca, Joanne Muir-Nash and Alfred D. Steinberg. "The Fatigue Severity Scale: Application to Patients with Multiple Sclerosis and Systemic Lupus Erythematosus." Arch Neurol 46 (1989): 1121-3.
[Crossref] [Google scholar] [pubmed]
- Ozyemisci-Taskiran, Ozden, Elif Balevi Batur, Selcen Yuksel and Mustafa Cengiz, et al. "Validity and Reliability of Fatigue Severity Scale in Stroke." Top Stroke Rehabil 26 (2019): 122-7.
[Crossref] [Google scholar] [pubmed]
- Schow, Trine, Thomas William Teasdale, Kirsten Jensen Quas and Morten Arendt Rasmussen. "Problems with Balance and Binocular Visual Dysfunction are associated with Post-stroke Fatigue." Top Stroke Rehabil 24 (2017): 41-9.
[Crossref] [Google scholar] [pubmed]
- Al-Rajeh, Saad, Adesola Ogunniyi, Adnan Awada and Abdulkader Daif, et al. "Preliminary Assessment of an Arabic Version of the Mini-Mental State Examination." Ann Saudi Med 19 (1999): 150-2.
[Crossref] [Google scholar] [pubmed]
- Amtmann, Dagmar, Alyssa M. Bamer, Vanessa Noonan and Nina Lang, et al. "Comparison of the Psychometric Properties of Two Fatigue Scales in Multiple Sclerosis." Rehabil Psychol 57 (2012): 159-66.
[Crossref] [Google scholar] [pubmed]
- Ponchel, Amélie, Stéphanie Bombois, Régis Bordet and Hilde Hénon. "Factors Associated with Poststroke Fatigue: A Systematic Review." Stroke Res Treat 2015 (2015): 347920.
[Crossref] [Google scholar] [pubmed]
- Hinkle, Janice L., Kyra J. Becker, Jong S. Kim and Smi Choi-Kwon, et al. "Poststroke Fatigue: Emerging Evidence and Approaches to Management: A Scientific Statement for Healthcare Professionals from the American Heart Association." Stroke 48 (2017): e159-e170.
[Crossref][Google scholar] [pubmed]
- Thilarajah, Shamala, Benjamin F. Mentiplay, Kelly J. Bower and Dawn Tan, et al. "Factors Associated with Post-stroke Physical Activity: A Systematic Review and Meta-analysis." Arch Phys Med Rehabil 99 (2018): 1876-89.
[Crossref] [Google scholar] [pubmed]
- Schepers, Vera P., Anne M. Visser-Meily, Marjolijn Ketelaar and Eline Lindeman. "Poststroke Fatigue: Course and its Relation to Personal and Stroke-related Factors." Arch Phys Med Rehabil 87 (2006): 184-8.
[Crossref] [Google scholar] [pubmed]
- Vincent-Onabajo, Grace and Abdulbaqi Adamu. "Prevalence of Post Stroke Fatigue among Stroke Survivors in Rehabilitation at Physiotherapy Facilities in Nigeria."
J Med Res 2 (2016): 32-4. [Crossref] - Duncan, Fiona, Susan J. Lewis, Carolyn A. Greig and Martin S. Dennis, et al. "Exploratory Longitudinal Cohort Study of Associations of Fatigue after Stroke." Stroke 46 (2015): 1052-8.
[Crossref] [Google scholar] [pubmed]
- Staub, Fabienne and Julien Bogousslavsky. "Fatigue after Stroke: a Major but Neglected Issue." Cerebrovasc Dis 12 (2001): 75-81.
- Appelros, Peter. "Prevalence and Predictors of Pain and Fatigue after Stroke: A Population-Based Study." Int J Rehabil Res 29 (2006): 329-33.
[Crossref] [Google scholar] [pubmed]
- Park, Ji Young, Min Ho Chun, Si Hyun Kang and Jin A. Lee, et al. "Functional outcome in Poststroke Patients with or without Fatigue." Am J Phys Med Rehabil 88 (2009): 554-8.
[Crossref] [Google scholar] [pubmed]
- Snaphaan, L. J. A. E., S. Van der Werf and F‐E. de Leeuw. "Time Course and Risk factors of Post‐stroke Fatigue: A Prospective Cohort Study." Eur J Neurol 18 (2011): 611-7.
[Crossref] [Google scholar] [pubmed]
- Sarfo, Fred S., Patrick Berchie, Arti Singh and Michelle Nichols, et al. "Prevalence, Trajectory, and Predictors of Poststroke Fatigue among Ghanaians." J Stroke Cerebrovasc Dis 28 (2019): 1353-61.
[Crossref] [Google scholar] [pubmed]
- Becker, Kyra, Ruth Kohen, Richard Lee and Patricia Tanzi, et al. "Poststroke Fatigue: Hints to a Biological Mechanism." J Stroke Cerebrovasc Dis 24 (2015): 618-21.
[Crossref] [Google scholar][pubmed]
- Graber, Mathilde, Lucie Garnier, Gauthier Duloquin and Sophie Mohr, et al. "Association between Fatigue and Cognitive Impairment at 6 months in Patients with Ischemic Stroke treated with Acute Revascularization Therapy." Front Neurol 10 (2019): 931.
[Crossref] [Google scholar] [pubmed]
Citation: Zaki, Mennatallah O., Abdelrheem M. Zidan, Abdullrahman M. Mahmoud and Omar Sh. Ali, et al. “Post Stroke Fatigue Prevalence and its Correlation to the Functional Recovery.” Clin Schizophr Relat Psychoses 16S (2022). Doi:10.3371/CSRP.AADF.022822.
Copyright: © 2022 Ali AS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.